- AdventHealth
Elakkat Dharmaraj Gireesh, MD
Neurologist
AdventHealth Neuroscience Institute
Epilepsy is a central nervous system (neurological) disorder in which brain activity becomes abnormal, causing periods of unusual behavior, sensations, loss of awareness and sometimes convulsions. The long-term effects of epilepsy include injuries, increased intensity and frequency of seizures over time, and memory problems. There are around 3.4 million people with epilepsy nationwide, which is around 1% of the US population, and 30-35% of these patients have drug-resistant epilepsy (DRE).
Epilepsy surgery is an option for some of the patients whose seizure focus is established through presurgical evaluations. Identifying the seizure onset zone can be challenging, especially when the MRI is negative for any definite abnormality that can explain the seizures. In those scenarios, intracranial electroencephalography (EEG) monitoring is used as a strategy for identifying seizure onset zones, with either surface electrodes or with stereo EEG (sEEG). Stereo EEG is a minimally invasive procedure that helps the epileptologist to find the seizure onset zones. During the sEEG, small wires with contacts record electrical activity on the surface and deeper locations of the brain. Neurosurgeons will put these wires in the brain using a robotic operating surgery assistant (ROSA) in the operating room. ROSA enables the neurosurgeon to place the wires precisely and efficiently, thereby reducing the operating time and complications.
Patients with drug-resistant epilepsy can be treated with surgical strategies designed to remove the seizure onset zone or to disrupt the epileptic network. Currently, long-term seizure control after epilepsy surgery ranges from 34-56% for epilepsy arising from locations other than the temporal lobe. Failure of adequate control has been attributed to the inability in identifying the epileptogenic zone(s) and inadequate or inaccurate surgical interventions.
The surgical options for epilepsy patients include resection of the seizure onset zones, disconnection of the seizure onset zones, laser interstitial thermal therapy (also called laser ablation or LITT) or neurostimulation strategies (responsive neural stimulation or deep brain neurostimulation). LITT is a minimally invasive surgical option for people with drug-resistant epilepsy, mainly for those with focal epilepsy, who have seizures originating in one particular region of the brain. In this procedure, the surgeon navigates a laser wire toward the area in the person’s brain that is identified as the source of seizures, with magnetic resonance imaging (MRI) guidance. Once the laser wire is placed in the area of interest, heat energy from the laser wire is used to destroy the region.
We have been using the sEEG with robotic guidance and LITT in appropriately selected patients since 2014. The patients for this procedure were selected through the presurgical work-up, including scalp video EEG evaluation; MRI brain, including diffusion tensor imaging (DTI) sequences; attempted ictal single-photon emission computerized tomography (SPECT); positron emission tomography (PET); magnetoencephalography (MEG); and neuropsychological evaluation to localize the epileptogenic zones.
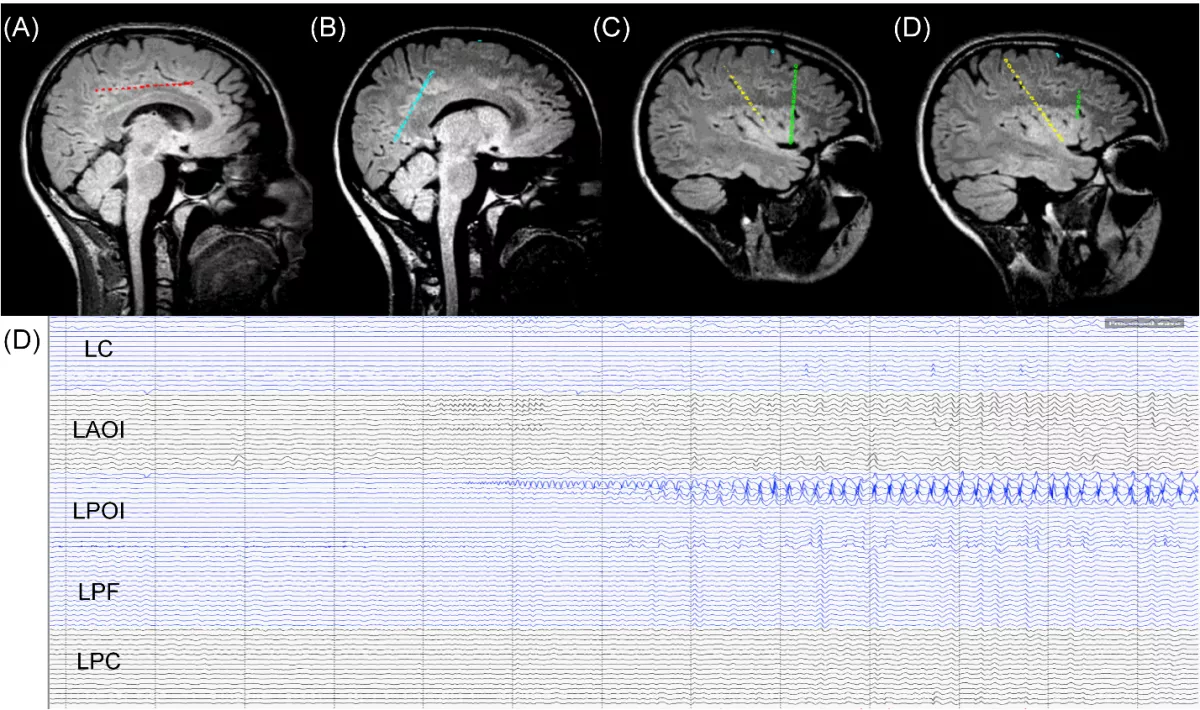
When insular or cingulate cortex are suspected as seizure onset zones, invasive monitoring of these structures with sEEG would improve epilepsy management. Neither the insula nor the cingulate can be easily monitored using subdural electrode arrays. Attempts to monitor these structures using combinations of subdural and depth electrodes have achieved inconsistent success in the past. Therefore, sEEG appears to be significantly helpful in localizing seizure onset zones in patients suspected to have insular and cingulate epilepsy.
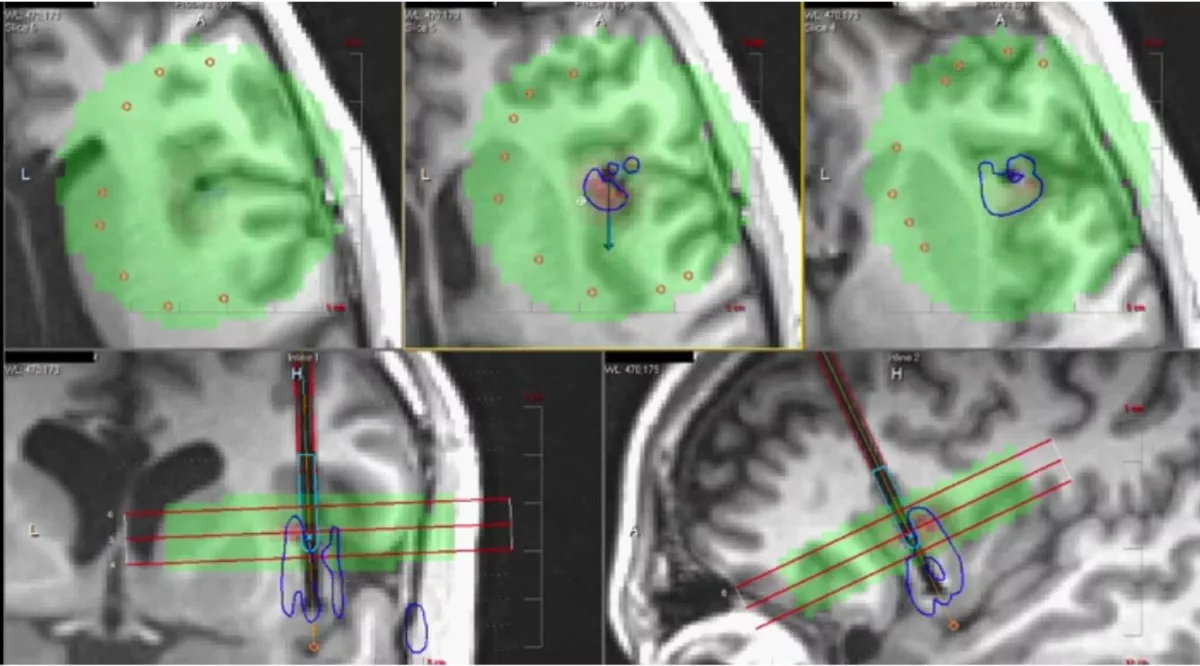
In the patients we reviewed in this study, sEEG electrodes were implanted with robotic guidance and monitored in the neuro intensive care unit (ICU) in order to capture typical seizures. Surgical intervention at insula or cingulate regions was recommended based on these evaluations. The fact that the insula lies deep within the sylvian fissure and is adjacent to critical structures, including the internal capsule, makes it difficult to approach using conventional surgical strategies. In the dominant hemisphere, the insula is covered by eloquent frontal, temporal and parietal opercula, and open surgery options in this region risks language impairment for the patient. The cingulate gyrus is challenging to access surgically because of its location along the deep medial surface of the brain. Given these challenges, LITT provides definite advantages for optimal interventions in these brain regions, minimizing the risks compared to an open surgery approach.
In our study involving the patients suspected of having insula and cingulate onset epilepsy who underwent intracranial monitoring and LITT of the insula and cingulum, 67% achieved complete seizure freedom, and all patients had a favorable response with worthwhile improvement in seizures. There were no permanent neurological or neuropsychological deficits in this group of patients. Hemorrhagic complications were noted in a small group of patients with no long-term sequelae. The complication rates associated with LITT in these locations were comparable to those following open insular resection. A dominant hemisphere insular or cingulate seizure onset zone is not a contraindication to LITT. Our experience suggests that sEEG followed by LITT is a reasonable treatment option for drug-resistant epilepsy originating from these difficult-to-access regions of the cerebral cortex, particularly for patients with non-lesional epilepsy. Potential risk of hemorrhage should be considered in the decision-making process.
Recent News

Historic telesurgery connects Central Florida and Angola in world-first medical breakthrough
AdventHealth’s Global Robotics Institute Sets New Standard in Remote Surgery

Empowering emerging women leaders
ATHENA NextGen’s Karen Keene joins AdventHealth’s Karen Corbin in a discussion about empowering the next wave of women leaders.
